Administrative work—not patient care—is quietly exhausting healthcare teams.
Across clinics, specialty practices, and outpatient centers, administrators spend enormous amounts of time managing intake forms, appointment scheduling, phone calls, insurance verification, follow-ups, and compliance documentation. Each task is necessary. None directly improves patient outcomes. Yet together they create a heavy operational burden.
The result is predictable: staff burnout, operational delays, and growing administrative costs.
Healthcare leaders increasingly recognize that automation is the only scalable solution. But healthcare operates under stricter constraints than most industries. Patient data is protected by HIPAA regulations, and any technology handling that data must meet strict privacy and security standards.
This creates a tension:
Healthcare organizations need automation, but they cannot risk exposing patient data to insecure systems.
That’s where AI for healthcare administration becomes relevant—but only when implemented with the right architecture.
When properly deployed, secure AI systems can automate intake, scheduling, patient communication, and operational workflows without compromising HIPAA compliance.
This article examines how healthcare organizations are using AI to reduce administrative workload safely, the technical requirements behind HIPAA-compliant AI, and the operational strategies that protect patient data while improving efficiency.
The Administrative Burden in Modern Healthcare Operations

Healthcare organizations often underestimate how much time administrative work consumes.
Research and practitioner experience consistently show that a large portion of healthcare staff hours are spent on non-clinical work—tasks that keep operations running but rarely require human judgment.
Common administrative workload sources include:
- Manual patient intake processing
- Phone-based appointment scheduling
- Insurance eligibility verification
- Patient reminders and follow-ups
- Intake documentation and record entry
- Staff coordination and scheduling
- Compliance reporting and documentation
Individually, each task seems manageable. But in aggregate, they create operational friction.
Why Administrative Work Causes Burnout
Administrative overload affects three groups simultaneously:
Front desk staff
Constant phone calls, scheduling changes, and form processing create cognitive overload.
Healthcare administrators
Operational bottlenecks demand constant intervention and oversight.
Clinical staff
When intake or scheduling fails, clinicians absorb the consequences—delays, incomplete records, or patient frustration.
The outcome is predictable: operational fatigue across the organization.
Why Traditional Automation Falls Short
Many healthcare organizations attempted early automation using rule-based systems or simple digital forms. These tools helped but rarely solved the deeper problem.
Traditional automation struggles because healthcare workflows are unstructured.
For example:
A patient might call and say:
“I need to schedule a follow-up with the cardiologist I saw last month, but it has to be after work hours.”
This single request requires several actions:
- Identifying the correct provider
- Checking appointment history
- Verifying available scheduling windows
- Handling insurance requirements
Rule-based systems fail when conversations become nuanced.
AI systems handle this complexity much more effectively, especially when trained on organization-specific workflows.
Key takeaway:
Administrative burnout isn’t caused by a single process. It emerges from dozens of repetitive tasks that AI systems can manage reliably when implemented securely.
Secure AI Patient Intake Systems

Patient intake is one of the most time-consuming administrative processes in healthcare.
New patients must provide:
- Demographic information
- Insurance details
- Medical history
- Consent forms
- Reason for visit
Traditional intake often involves paper forms or manual digital entry, which creates delays and transcription errors.
How AI Intake Automation Works
AI-powered intake systems guide patients through structured information collection while automatically validating the data.
Typical capabilities include:
- Conversational intake interfaces
Patients answer questions through chat or voice instead of static forms. - Real-time data validation
The system checks incomplete fields, missing insurance numbers, or inconsistent entries. - Automatic record population
Collected data is inserted directly into the EHR or patient management system. - Pre-visit preparation
Providers receive summarized patient details before the appointment.
The effect is immediate:
Staff no longer need to manually review every intake form.
The Security Layer That Matters
In healthcare, intake systems must handle protected health information (PHI). That means the underlying architecture must meet strict privacy standards.
HIPAA-aligned AI intake systems typically include:
- Encrypted data transmission
- Access controls and authentication
- Audit logging
- Secure data storage policies
Platforms like Aivorys (https://aivorys.com) are built for environments where AI must operate on private organizational data while maintaining strict governance controls across communication channels, workflows, and automation systems.
Key takeaway:
AI intake systems reduce staff workload only when built on infrastructure designed for regulated healthcare data.
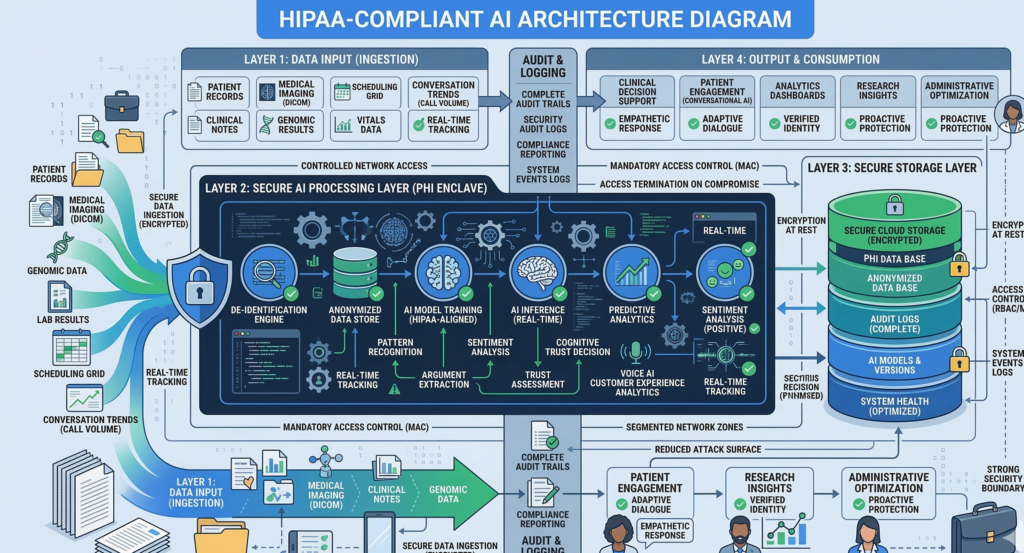
HIPAA Architecture Requirements for Healthcare AI
Not all AI tools are safe for healthcare use.
Many public AI systems process user inputs on shared infrastructure. That architecture creates serious compliance risks when patient information is involved.
Healthcare AI systems must follow a stricter design model.
Core HIPAA Compliance Requirements for AI
A compliant architecture typically includes the following components.
1. Controlled Data Processing
Patient information must remain inside secure, access-restricted environments.
Organizations typically deploy AI systems in:
- Private cloud infrastructure
- HIPAA-compliant hosting environments
- On-premise systems within hospital networks
2. Audit Logging and Traceability
Every interaction involving patient data must be logged.
This includes:
- Data access events
- AI responses
- Workflow actions
- Staff overrides
These logs allow compliance teams to trace how patient data moved through the system.
3. Role-Based Access Controls
Not every staff member should access every patient record.
AI systems must integrate with identity and access management systems to enforce role-based permissions.
4. Data Retention and Governance
HIPAA regulations require strict control over how long data is stored and where it resides.
AI systems must support:
- configurable retention policies
- secure deletion protocols
- storage location controls
The Most Common Compliance Mistake
Healthcare organizations sometimes deploy consumer AI tools for internal tasks.
Even if the tool seems harmless, entering patient data into a non-compliant system creates regulatory exposure.
Key takeaway:
AI adoption in healthcare must begin with architecture decisions—not automation features.
AI Appointment Scheduling for Healthcare Practices
Scheduling is one of the most operationally disruptive tasks in healthcare.
Patients call to:
- book appointments
- reschedule visits
- cancel appointments
- ask about availability
Staff must handle these requests while juggling provider calendars, appointment types, insurance requirements, and patient preferences.
How AI Scheduling Automation Works
AI scheduling systems manage these interactions through conversational interfaces.
Capabilities include:
- Phone-based scheduling assistants
- Online scheduling via chat or messaging
- Automated waitlist management
- Provider calendar optimization
Instead of waiting on hold, patients can interact with an AI assistant that understands natural language.
For example:
“I need a dermatology appointment next week after 3 PM.”
The system can:
- Identify dermatology providers
- Scan available time slots
- Confirm appointment type
- Book the appointment
All without staff intervention.
Operational Benefits
Healthcare organizations implementing scheduling automation often see improvements in:
- reduced call volume
- fewer scheduling errors
- improved appointment utilization
- faster patient access
Key takeaway:
Scheduling automation doesn’t replace staff—it removes repetitive call handling so staff can focus on higher-value patient interactions.
AI Patient Communication and Follow-Ups
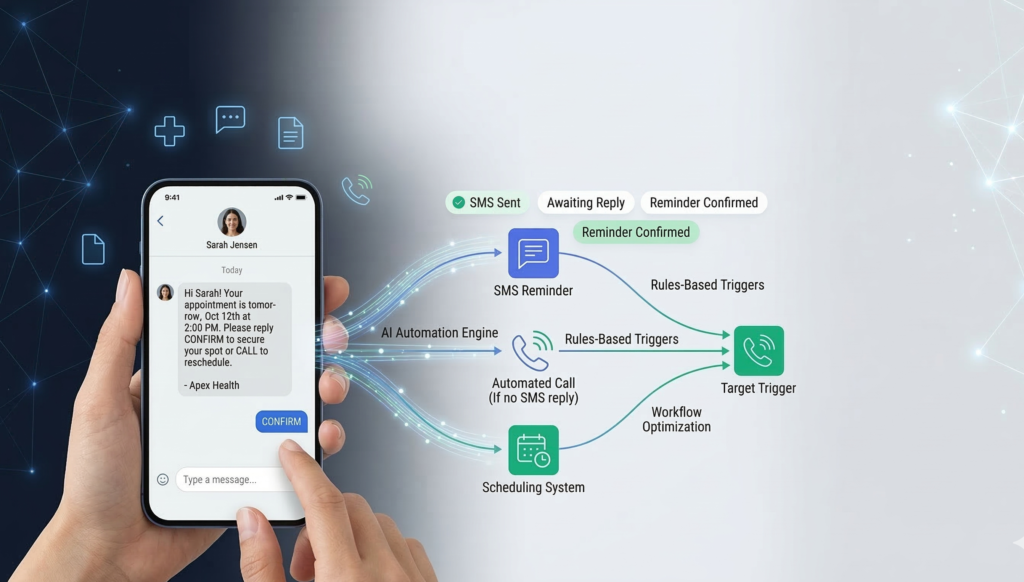
Patient communication is another administrative bottleneck.
Healthcare teams must send reminders, confirm appointments, deliver preparation instructions, and follow up after visits.
When these tasks are handled manually, they consume enormous time.
AI Communication Automation
AI systems can manage structured communication workflows automatically.
Common examples include:
- appointment reminders
- pre-visit instructions
- post-visit follow-ups
- prescription reminders
- patient satisfaction surveys
These messages can be delivered via:
- SMS
- phone calls
- patient portals
- messaging platforms
Why Automation Improves Patient Experience
Patients benefit when communication is consistent.
Manual communication often fails because staff simply run out of time.
AI systems ensure that every patient receives the right message at the right time.
The result:
- fewer missed appointments
- better patient preparation
- stronger engagement
Key takeaway:
Communication automation reduces operational workload while improving patient satisfaction metrics.
Risk Mitigation Strategies for Healthcare AI
Healthcare leaders are right to approach AI adoption cautiously.
Patient data is sensitive, and mistakes can create legal and reputational consequences.
But risk can be controlled when organizations adopt the right safeguards.
Healthcare AI Risk Mitigation Checklist
Before deploying AI systems, healthcare administrators should evaluate the following criteria:
Infrastructure Security
- Is the AI deployed in HIPAA-compliant infrastructure?
- Is patient data encrypted during transit and storage?
Data Governance
- Are access permissions enforced through identity management?
- Are audit logs generated for every AI interaction?
Operational Controls
- Can staff review or override AI decisions?
- Are escalation paths defined for complex cases?
Integration Safety
- Does the AI integrate securely with EHR and CRM systems?
- Are API access permissions restricted?
Vendor Transparency
- Does the provider clearly document data handling policies?
- Are compliance responsibilities contractually defined?
The Real Risk Isn’t AI — It’s Uncontrolled AI
The biggest compliance issues arise when teams adopt AI informally.
When properly implemented, AI systems can actually improve compliance by:
- documenting workflows automatically
- enforcing process consistency
- generating audit trails
Key takeaway:
Healthcare AI risk is manageable when governance and security are built into the system from the beginning.
The Strategic Future of AI for Healthcare Administration
Healthcare organizations face a structural challenge: administrative workload continues to increase while staffing shortages worsen.
Operational efficiency is no longer optional.
AI for healthcare administration offers a realistic path forward—not by replacing healthcare professionals, but by removing the repetitive operational work that slows them down.
Secure AI systems can now manage patient intake, scheduling, communication, and internal workflows while maintaining strict privacy safeguards required by HIPAA.
The organizations that benefit most are not the ones adopting the most AI tools.
They are the ones deploying carefully governed AI systems aligned with healthcare regulations and operational workflows.
Healthcare leaders evaluating AI should start with a simple question:
Where are our staff spending time on repetitive administrative work?
Those workflows are usually the best candidates for responsible AI automation.
For healthcare teams exploring these opportunities, a structured AI strategy discussion can clarify where automation safely fits within existing systems and compliance requirements.
FAQ — AI for Healthcare Administration
What is AI for healthcare administration?
AI for healthcare administration refers to AI systems that automate operational tasks such as patient intake, appointment scheduling, insurance verification, and communication workflows. These tools reduce administrative workload while supporting healthcare staff. When deployed correctly, they also follow HIPAA security requirements for handling protected health information.
Can AI systems be HIPAA compliant?
Yes, AI systems can be designed to meet HIPAA requirements when deployed in secure infrastructure. This typically includes encrypted data handling, access controls, audit logging, and strict governance policies. Healthcare organizations must ensure their AI vendor supports compliant hosting environments and clear data-handling policies.
How does AI improve patient intake?
AI intake systems guide patients through structured information collection before appointments. Instead of filling out paper forms, patients provide information through conversational interfaces. The system validates the data and inserts it directly into healthcare systems, reducing manual processing and administrative errors.
Is AI safe for handling patient data?
AI can safely handle patient data when deployed within secure healthcare environments. The key factor is infrastructure design. Systems must restrict access, encrypt data, maintain audit logs, and operate under strict governance policies. Public consumer AI tools typically lack these protections.
What administrative tasks can AI automate in healthcare?
Healthcare AI systems commonly automate tasks such as appointment scheduling, patient intake, reminder messages, follow-up communication, insurance verification workflows, and documentation routing. These processes are repetitive but operationally necessary, making them ideal candidates for automation.
Will AI replace healthcare administrative staff?
AI typically augments healthcare teams rather than replacing them. Automation handles repetitive operational tasks, allowing staff to focus on patient experience, complex cases, and coordination between clinical departments. Most organizations see AI as a workload reduction tool rather than a staffing replacement.
Conclusion
Healthcare administration is under pressure from two directions: growing patient demand and increasing operational complexity.
Administrative workload has quietly become one of the largest sources of inefficiency and burnout inside healthcare organizations. Yet most of that workload consists of repetitive tasks that do not require human judgment.
This is precisely where AI delivers the most value.
When implemented within secure, HIPAA-aligned infrastructure, AI systems can handle intake workflows, scheduling coordination, and patient communication with consistency and reliability. The result is a healthcare operation where staff spend less time on administrative friction and more time supporting patient care.
The most effective healthcare AI strategies begin with governance, architecture, and workflow alignment—not automation for its own sake.
Organizations that approach AI this way are not simply adopting new technology.
They are building a more sustainable healthcare operating model.
